Introduction
Jasmine, rose, and sandalwood; these are the scents that permeate my childhood memories. From the burning of incense sticks to the steady stream of fragrances coming from my essential oil diffuser, this is how I know I’m home – something that you may be familiar with as “aromatherapy”, the use of aromatic materials to enhance psychological and physical well-being.
Aside from serving as a non-toxic way to make your house smell good, aromatherapy can be used as a complementary and alternative medicine (CAM) practice, which encompasseses non-traditional medical therapies such as acupuncture, aromatherapy, or homeopathy. Aromatherapy uses essential oils, which are concentrated aromatic compounds naturally extracted from the oil sacs of anything ranging from flowers and seeds to fruits and rinds. Once these volatile oils are extracted, the two most common methods of usage are through diffusion and massage. Aromatherapy has ample uses both recreationally and clinically, whether it be by making your room smell of your favorite flowers or helping fight against overactive enzymes that contribute to Alzheimer’s disease [1].
However, in some realms of medicine, particularly Western medicine, there tends to be skepticism towards CAM procedures such as aromatherapy. As a result, aromatherapy is usually dismissed as a pseudoscience, since the field is currently lacking in comprehensive clinical research assessing the effects of such therapies [2]. In more recent years, however, the research community has reopened this conversation, making efforts to re-examine CAM procedures that were previously dismissed. While there has yet to be sufficient evidence indicating that the practice can serve as a standalone treatment for most medical conditions, researchers have discovered numerous positive effects that aromatherapy has on our brains both on its own and in tandem with other treatments. This indicates that such therapies can hold numerous physiological and psychological benefits, especially when used with other forms of treatment [2].
Aromatherapy and the Brain
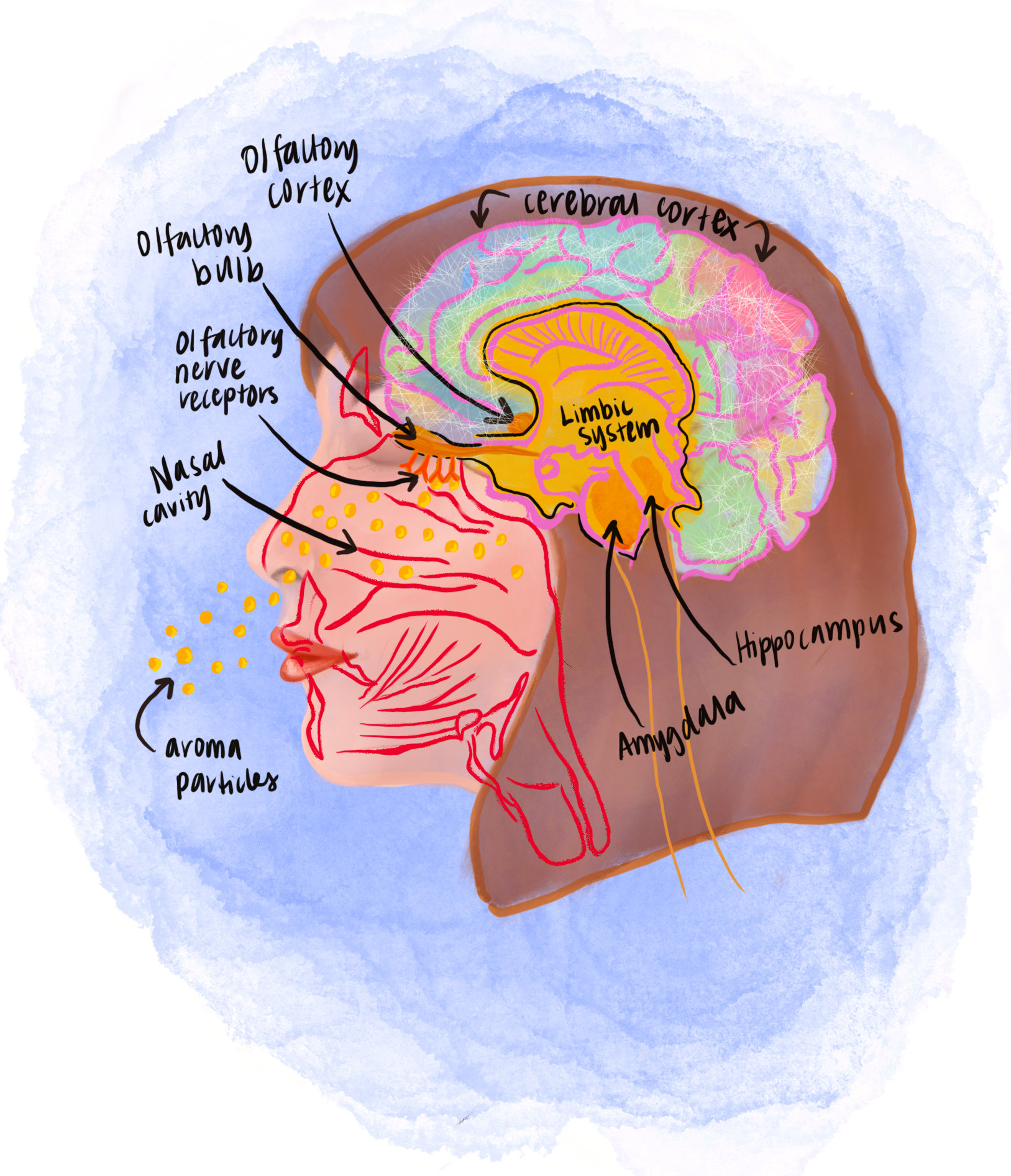
One of the primary reasons why aromatherapy can affect our brain is due to the unique relationship between our brain and sense of smell. Inhaled essential oil molecules activate neural signaling in the olfactory bulb, the region of the brain that captures and sends out information regarding smell. This stimulus then travels to the limbic system of the brain, a region that regulates emotion and cognition - specifically to the amygdala and hippocampus. These two limbic structures that are responsible for forming emotional responses and memory encoding, respectively. The limbic system then interacts with the cerebral cortex, which activates specific thoughts, feelings, and actions, and the olfactory cortex receives nerve signals that trigger the release of neurotransmitters such as serotonin [2].
Olfaction and the limbic system are incredibly intertwined; in fact, smell is the only sense that bypasses processing in the thalamus, the region of the brain that processes information gained from all our other senses except smell. Instead, stimuli from scents go straight to the olfactory bulb, which is directly connected to the limbic system, and thus olfactory perception is dominated by an emotional response to the scent. For example, you may be more likely to remember that your dirty socks “smell bad” rather than what exactly they smell like [3]. The close interaction between our brain and scent is what allows smells to strongly trigger certain emotions and memories compared to our other senses, even inducing calming, stress-relieving effects on our minds [4].

Aromatherapy and the Mind
Lavender, chamomile, and bergamot; these three words may evoke various different scents and images - a steaming cup of chamomile tea before bedtime, a stroll through one of Washington’s various lavender fields, or the smell of fresh-squeezed citruses. But beyond that, these are also some of the essential oils shown to have significant psychological effects on the brain and are often used to aid treatment of mental disorders such as anxiety, depression, or insomnia.
Lavender essential oil is one of the most popular and versatile essential oils - it’s likely that you’re familiar with the scent, perhaps through candles, soaps, or perfumes. However, the oil also has purposes beyond cosmetic, such as management of anxiety and pain perception. A study conducted on burn patients in 2016 showed that aromatherapy inhalation and massage significantly reduced the pain and anxiety of these patients [5]. The randomized clinical trial assigned patients to either the aromatherapy massage group, aromatherapy inhalation group, or control group (no therapy). Post-treatment patient responses using the Spielberger State Anxiety Inventory, a 40 question survey used for evaluating patient anxiety levels from 0-3 points for each question, showed that patients who received the aromatherapy massage or inhalation treatment had reduced anxiety levels by an average of 6.33 and 6.43 points on the scale respectively, compared to an increase anxiety by 0.04 points for the control group. Pain responses using the visual analogue scale, a questionnaire for gauging pain level, showed that patients who received aromatherapy massage or inhalation treatments experienced a reduction in pain perception by 1.7 and 0.97 points on the scale respectively, compared to an increase in pain perception by -0.1 for the control group [5].
Additionally, another similar study on burn patients was done in 2019 with essential oil from the chamomile flower along with lavender essential oil [6]. The study randomly assigned burn patients to control, placebo, and aromatherapy massage groups (which used a blend of chamomile and lavender essential oil), and showed similar results to the previous study using the Spielberg State Anxiety Inventory and the Pittsburgh Sleep Quality Inventory. Before the treatment, patients in all three groups did not have significant differences in anxiety or sleep quality scores, whereas after treatment, patients in the aromatherapy massage group were statistically shown to have significantly lower anxiety scores and significantly higher sleep quality scores [6].
While the studies done with burn patients showcase the psychological potential of lavender and chamomile essential oil in regulating pain and anxiety, it’s important to understand what might be occurring here at the molecular level. A 2017 study showed that lavender essential oil has significant effects on the central nervous system (CNS), which comprises the brain and spinal cord. Use of the oil increases the release of chemicals such as serotonin, GABA, and NMDA [7]. Often called the “happy neurotransmitter”, serotonin is involved in regulation of mood, memory, and learning; depression medication such as SSRIs (Selective Serotonin Reuptake Inhibitors) thus increase the activation of serotonin receptors. GABA is a neurotransmitter that makes neurons less excitable, and thus often used in anti-anxiety and anticonvulsant medication. NMDA is a receptor system that regulates learning and neuroplasticity, which refers to our brain’s ability to form/reorganize neural pathways based on learning new skills, psychological stress, and various other experiences - therefore, manipulation of NMDA receptors can help alleviate neurodegenerative symptoms. The researchers in the study used bioassays, a method to determine the potency of a substance through measurable effects it has on a living system, in this case to test lavender essential oil on tissue from rat brains [8]. The high affinity that lavender essential oil and its compounds show for serotonin transporters, GABA receptors, and NMDA receptors show that this oil could potentially be used in treatment of CNS disorders such as anxiety and stress [8].
Bergamot essential oil (BEO) also holds potential to be used clinically in treatments of mental disorders, similar to lavender or chamomile essential oil. A 2019 study found that BEO served as an anxiolytic (reducing anxiety levels) in rats, with pharmacological effects similar to common anti-anxiety medications [9]. Researchers conducted a variety of behavioral trials such as running through a maze, swimming, and open field tests to compare the rats under the effects of bergamot oil and no treatment. Under BEO treatment, the rats exhibited lower frequency of wallrearing, which is to touch the walls of the maze with their forelimbs, and increased frequency of immobility while swimming, showing that bergamot essential oil has behavioral anxiolytic and relaxant/sedative effects in the mice. This effect may be owed to bergamot essential oil’s ability to stimulate release of GABA and glutamate - a neurotransmitter that works together with GABA to regulate the brain’s level of excitement - and thus inducing a similar effect as lavender essential oil [10]. They may be small, but the compounds in these essential oils are mighty in the way they can influence the way our brain processes emotions, potentially helping manage symptoms of anxiety, stress, and physical pain.
Aromatherapy in Medical Research
Mint, sage, and rosemary; hearing the names of these common herbs may bring certain flavors and scents to mind, such as the aftertaste of toothpaste after brushing your teeth in the morning, or the scent of rosemary chicken cooking. But the effects the essential oils of these herbs have on the brain serve as examples of how aromatherapy can affect our brains to induce systemic effects such as inhibiting the production of the enzyme acetylcholinesterase, which breaks down the neurotransmitter acetylcholine, or improving the personal orientation of Alzheimer’s patients [11].
Rosemary may have powerful uses outside the kitchen, such as therapeutic potential for Alzheimer’s Disease patients [11]. A clinical study done on Alzheimer’s patients in Japan showed that after receiving aromatherapy treatment of lavender and rosemary essential oil blends, they experienced an increase in abstract and cognitive function. After a 28 day control period, the patients received aromatherapy treatment through diffusion for 28 days. This was followed by another 28 day washout period in which the patients received no treatment, in order to serve as a post-intervention control. Then, cognitive function of patients was evaluated using the Touch Panel-type Dementia Assessment Scale (TDAS), a method which quickly evaluates the severity of cognitive dysfunction symptoms by using various tests such as word-recognition and following commands, as well as the Gottfries-Brane-Steen Scale (GBSS-J), a method employing observation and interviews with patients to measure their intellectual and emotional symptoms of dementia [12][13]. The results showed that using the TDAS, improvements in cognitive function were noted for all patients, whereas the subsections of cognitive function and spontaneity were observed using the GBSS-J [11].
Let’s take a look at what could potentially be occurring here at the molecular level. Essential oils from the mint family, Lamiaceae (including mint, lavender, sage, basil, rosemary, and more), contain a high percentage (90%) of monoterpenes [14], which are a class of molecules small enough to cross the highly selective and semi-permeable blood brain barrier (BBB) [15]. Since essential oils are mostly made of small, fat soluble organic molecules, they can usually cross the BBB and interact with general neural circuitry of the CNS by influencing the production of enzymes involved in the regulation of neurotransmitters/neurotransmission [16].
Research published in 2019 showed that certain monoterpenoids from Lamiaceae essential oils have inhibitory effects on an enzyme called acetylcholinesterase both in vivo (studies performed on living organisms) and in vitro (studies performed outside a living organism) [1]. Acetylcholinesterase is an enzyme that breaks down acetylcholine, a neurotransmitter that is key in modulating synaptic transmission in the CNS. In this context, it plays a significant role in the processing of information and memories and is thus linked with Alzheimer’s disease, the most common form of dementia [17]. Patients with Alzheimer’s have excess amounts of the acetylcholinerase enzyme and thus not enough acetylcholine. The current standard treatment of Alzheimer’s uses acetylcholinerase inhibitors, with which certain essential oils have similar inhibitory effects [18].
In order to test the effects of these essential oils on acetylcholinesterase, the researchers used a method known as high-performance thin-layer chromatography (HPTLC) [1]. HPTLC is a method used to separate volatile compounds from non-volatile ones and test their properties. Enzyme activity was detected by the reaction of the molecules with the dye,and inhibitors of acetylcholinesterase produced white spots on the purple dye-coloured background on the TLC plates. From these assays, the researchers determined that sage essential oil had significantly high acetylcholinesterase inhibitory activity, which was higher than other essential oils in the family. Given the biological effects these essential oils can have and their ability to cross the blood brain barrier, usage of these essential oils may have potential to help boost cognitive function and reduce the severity of diseases like Alzheimer’s [1].
The Limitations and Future of Aromatherapy
Despite the psychological and physiological benefits that aromatherapy may come with, it is not without its limitations. For example, we currently do not have enough information about the specific physiological effects that different essential oils can trigger and how mixing different essential oils may amplify these effects. Methods such as QSAR (Quantitative Structure Activity Relationships) computationally model chemical compounds to reveal relationships between their structural and biological interactions. This method can be used to better predict BBB permeability for different essential oil compounds and discover which compounds can most effectively induce systemic effects, and in what combinations [1]. Conducting more research on the specific physicochemical properties of these compounds in clinical settings (rather than in vitro or using animal models as many of the current studies do) will also allow us to understand whether they have any potential targeted therapeutic effects on humans, such as the inhibitory effect essential oils from the mint family could have on acetylcholinesterase. With further research, using essential oils in tandem with other therapies can be a non-toxic, holistic, and targeted approach to reduce the intensity of the negative side effects and symptoms that more traditional medicines and therapies may cause, such as pain and nausea in chemotherapy patients [19] [20].
Aromatherapy has countless uses, both explored and unexplored. Due to the tiny yet mighty compounds that essential oils are made up of which give it BBB permeability, the same herb you may use to season your potatoes (sage) could help inhibit acetylcholinesterase in Alzhemier’s patients, or the same flower used to scent your deodorant (lavender) may help manage symptoms of mental disorders such as anxiety and depression. The further we research the neurobiological effects of this therapy and how it affects our body and brain, the closer we are to fully harnessing its potential and our brain’s extraordinary relationship with scent.
References
- Agatonovic-Kustrin, S., Kustrin, E., & Morton, D. W. (2019). Essential oils and functional herbs for healthy aging. Neural regeneration research, 14(3), 441–445. https://doi.org/10.4103/1673-5374.245467
- Farrar, A. J., & Farrar, F. C. (2020). Clinical Aromatherapy. The Nursing clinics of North America, 55(4), 489–504. https://doi.org/10.1016/j.cnur.2020.06.015
- Krusemark, E. A., Novak, L. R., Gitelman, D. R., & Li, W. (2013). When the sense of smell meets emotion: anxiety-state-dependent olfactory processing and neural circuitry adaptation. The Journal of neuroscience : the official journal of the Society for Neuroscience, 33(39), 15324–15332. https://doi.org/10.1523/JNEUROSCI.1835-13.2013
- Smith TD, Bhatnagar KP. Anatomy of the olfactory system. Handb Clin Neurol. 2019;164:17-28. doi: 10.1016/B978-0-444-63855-7.00002-2. PMID: 31604545.
- Seyyed-Rasooli A, Salehi F, Mohammadpoorasl A, Goljaryan S, Seyyedi Z, Thomson B. Comparing the effects of aromatherapy massage and inhalation aromatherapy on anxiety and pain in burn patients: A single-blind randomized clinical trial. Burns. 2016 Dec;42(8):1774-1780. doi: 10.1016/j.burns.2016.06.014. Epub 2016 Aug 27. PMID: 27575673.
- Rafii F, Ameri F, Haghani H, Ghobadi A. The effect of aromatherapy massage with lavender and chamomile oil on anxiety and sleep quality of patients with burns. Burns. 2020 Feb;46(1):164-171. doi: 10.1016/j.burns.2019.02.017. Epub 2019 Dec 16. PMID: 31859096.
- Garland E. L. (2012). Pain processing in the human nervous system: a selective review of nociceptive and biobehavioral pathways. Primary care, 39(3), 561–571. https://doi.org/10.1016/j.pop.2012.06.013
- López, V., Nielsen, B., Solas, M., Ramírez, M. J., & Jäger, A. K. (2017). Exploring Pharmacological Mechanisms of Lavender (Lavandula angustifolia) Essential Oil on Central Nervous System Targets. Frontiers in pharmacology, 8, 280. https://doi.org/10.3389/fphar.2017.00280
- Rombolà, L., Tridico, L., Scuteri, D., Sakurada, T., Sakurada, S., Mizoguchi, H., Avato, P., Corasaniti, M. T., Bagetta, G., & Morrone, L. A. (2017). Bergamot Essential Oil Attenuates Anxiety-Like Behaviour in Rats. Molecules (Basel, Switzerland), 22(4), 614. https://doi.org/10.3390/molecules22040614
- Scuteri, D., Rombolà, L., Morrone, L. A., Bagetta, G., Sakurada, S., Sakurada, T., Tonin, P., & Corasaniti, M. T. (2019). Neuropharmacology of the Neuropsychiatric Symptoms of Dementia and Role of Pain: Essential Oil of Bergamot as a Novel Therapeutic Approach. International journal of molecular sciences, 20(13), 3327. https://doi.org/10.3390/ijms20133327
- Jimbo D, Kimura Y, Taniguchi M, Inoue M, Urakami K. Effect of aromatherapy on patients with Alzheimer's disease. Psychogeriatrics. 2009 Dec;9(4):173-9. doi: 10.1111/j.1479-8301.2009.00299.x. PMID: 20377818.
- Inoue M, Jimbo D, Taniguchi M, Urakami K. Touch Panel-type Dementia Assessment Scale: a new computer-based rating scale for Alzheimer's disease. Psychogeriatrics. 2011 Mar;11(1):28-33. doi: 10.1111/j.1479-8301.2010.00345.x. Epub 2011 Feb 25. PMID: 21447106.
- Bråne G, Gottfries CG, Winblad B. The Gottfries-Bråne-Steen scale: validity, reliability and application in anti-dementia drug trials. Dement Geriatr Cogn Disord. 2001 Jan-Feb;12(1):1-14. doi: 10.1159/000051230. PMID: 11125236.
- Hajdari A, Mustafa B, Hyseni L, Bajrami A, Mustafa G, Quave CL, Nebija D. Phytochemical Study of Eight Medicinal Plants of the Lamiaceae Family Traditionally Used as Tea in the Sharri Mountains Region of the Balkans. The Scientific World Journal. 2020 Feb. https://doi.org/10.1155/2020/4182064
- Zhang Y, Long Y, Yu S, Li D, Yang M, Guan Y, Zhang D, Wan J, Liu S, Shi A, Li N, Peng W. Natural volatile oils derived from herbal medicines: A promising therapy way for treating depressive disorder. Pharmacol Res. 2021 Feb;164:105376. doi: 10.1016/j.phrs.2020.105376. Epub 2020 Dec 11. PMID: 33316383.
- Agatonovic-Kustrin S, Chan CKY, Gegechkori V, Morton DW. Models for skin and brain penetration of major components from essential oils used in aromatherapy for dementia patients. J Biomol Struct Dyn. 2020 May;38(8):2402-2411. doi: 10.1080/07391102.2019.1633408. Epub 2019 Jun 23. PMID: 31204906.
- Gale SA, Acar D, Daffner KR. Dementia. Am J Med. 2018 Oct;131(10):1161-1169. doi: 10.1016/j.amjmed.2018.01.022. Epub 2018 Feb 6. PMID: 29425707.
- Saxena M, Dubey R. Target Enzyme in Alzheimer's Disease: Acetylcholinesterase Inhibitors. Curr Top Med Chem. 2019;19(4):264-275. doi: 10.2174/1568026619666190128125912. PMID: 30706815.
- Evans A, Malvar J, Garretson C, Pedroja Kolovos E, Baron Nelson M. The Use of Aromatherapy to Reduce Chemotherapy-Induced Nausea in Children With Cancer: A Randomized, Double-Blind, Placebo-Controlled Trial. J Pediatr Oncol Nurs. 2018 Nov/Dec;35(6):392-398. doi: 10.1177/1043454218782133. Epub 2018 Jun 27. PMID: 29947285.
- Ramsey JT, Shropshire BC, Nagy TR, Chambers KD, Li Y, Korach KS. Essential Oils and Health. Yale J Biol Med. 2020 Jun 29;93(2):291-305. PMID: 32607090; PMCID: PMC7309671.
